Dental implants rely on solid bone support. Without enough healthy bone, the implant loses stability, the restoration fails prematurely, and long-term results suffer. At JP Prosthodontics in Fullerton, CA, bone quality and volume sit at the center of every implant treatment plan, especially in complex or full arch cases.
This guide explains why bone matters, when bone grafting becomes necessary, and how a prosthodontist and surgical team coordinate care to secure a stable foundation for implants.
Why Jawbone Shrinks After Tooth Loss
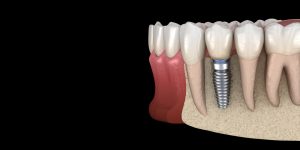
Tooth roots deliver mechanical stimulation to the jawbone during chewing. Once a tooth is removed, the bone in that area stops receiving regular load. The body responds by resorbing, or shrinking, the unused bone.
Patterns of bone loss:
- Fastest in the first 6–12 months after extraction
- Gradual but continuous over the following years
- Often more severe in long-term denture wearers
- More pronounced in thin, delicate ridges
Shrinking bone reduces support for dentures and makes implant placement more complex. Restoring missing teeth with dental implants in Fullerton helps interrupt this process by placing new “roots” into the bone and re-establishing stimulation.
How Bone Volume Affects Implant Planning
Implant stability depends on having enough bone height, width, and density. Before recommending implant treatment, JP Prosthodontics evaluates:
- Vertical height of bone near sinuses in the upper jaw
- Horizontal thickness of bone at planned implant sites
- Proximity to nerves and adjacent teeth
- Presence of defects, old infection sites, or traumatic loss
- Overall pattern of resorption from long-term tooth loss or denture wear
Cone beam CT imaging provides a 3D view of the jaw, allowing precise measurement and planning. If the bone falls below safe thresholds, bone grafting becomes part of the plan rather than an afterthought.
What Bone Grafting Is in Practical Terms
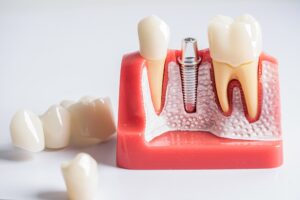
Bone grafting adds or rebuilds bone in areas where it is too thin or short to securely hold an implant. It does not replace the implant; it prepares the site so the implant can anchor properly.
Typical sources and materials:
- Processed donor bone
- Synthetic graft materials designed to support new bone formation
- The patient’s own bone in select cases
Common grafting goals:
- Increase ridge width to allow proper implant diameter
- Regain vertical height near sinuses or nerve canals
- Repair defects from previous infections, extractions, or trauma
- Create a stable, continuous ridge for full arch implant solutions
Graft material acts as a scaffold. Over time, the body replaces it with new, living bone, ready to integrate with titanium implants.
Types of Bone Grafting Used With Dental Implants
Several grafting approaches support different clinical situations.
Socket Preservation
Performed immediately after extraction.
- The socket is cleaned and filled with graft material.
- A membrane or covering may be placed to protect the area.
- The goal is to maintain ridge shape and volume during healing.
Socket preservation helps reduce the amount of bone loss that usually follows an extraction and often simplifies future implant placement.
Ridge Augmentation
Used when the ridge is already thin, flat, or significantly resorbed.
- Graft material is placed along the deficient area.
- Membranes and sutures protect and stabilize the graft.
- Healing takes several months before implants can be placed.
Ridge augmentation creates enough width and height for predictable implant placement, especially in cosmetically critical areas.
Sinus Lift (Sinus Augmentation)
Used in the upper back jaw when sinus expansion reduces bone height.
- A small window is created in the sinus wall.
- The sinus membrane is gently lifted.
- Graft material is placed underneath the membrane to increase bone height.
After healing, implants can be placed into the newly augmented area.
When Bone Grafting Is Usually Recommended
Bone grafting becomes part of the treatment plan when:
- The jawbone is too thin or short for standard implant placement.
- Long-standing missing teeth have led to severe ridge resorption.
- Full arch or full mouth dental implants require a continuous, stable foundation.
- The sinus floor has dropped into the space where upper back teeth used to be.
- Defects from infection, cysts, or trauma leave irregular bone contours.
Grafting is not used in every case. Some patients retain sufficient bone and move directly to implant placement. Others need only minor augmentation. Complex cases may require staged grafting and healing periods before the final implant plan proceeds.
Coordination Between Prosthodontics and Oral Surgery
Implant success depends on alignment between the restorative plan and surgical execution. JP Prosthodontics coordinates closely with the surgical team so the final tooth position drives implant and graft placement, not the other way around.
Key steps in coordinated planning:
- Defining the ideal tooth position, shape, and bite in advance
- Using 3D imaging and digital planning to map implant locations backward from the prosthetic design
- Determining where and how much grafting is required to support those positions
- Using surgical guides to transfer the digital plan accurately to the mouth
This approach keeps the outcome focused on function, aesthetics, and long-term health rather than only on placing implants wherever bone happens to be available.
Healing Timelines for Bone Grafting and Implants
Healing times vary depending on graft type, patient health, and the size of the grafted area. General patterns:
- Socket preservation: often 3–4 months before implant placement
- Ridge augmentation: typically 4–6 months of healing
- Sinus lift: frequently 6 months or longer before implants reach full stability
In some cases, implants are placed at the same time as smaller grafts. In larger or more complex grafts, staging the procedures produces more predictable long-term results. The oral surgery services page outlines broader surgical capabilities that support this type of structured, stepwise treatment.
Bone Grafting and Full Arch Implant Solutions
Full arch and full mouth treatments place higher demands on bone volume and distribution than single implants. The implant-supported prosthesis must handle all chewing forces across the arch.
Role of grafting in full arch cases:
- Creating sufficient bone for multiple implants across the jaw
- Equalizing support on both sides of the arch
- Avoiding anatomical structures while still achieving stable distribution
- Maintaining facial contours and lip support for an esthetic outcome
When needed, grafting becomes part of a phased plan that may start with extractions, temporary prostheses, and bone building, then progress to definitive full arch implant placement and final restorations.
Factors That Influence Graft Success
Several variables affect how well a graft integrates and supports future implants:
- Overall health and healing capacity
- Control of systemic conditions such as diabetes
- Smoking status and vascular health
- Oral hygiene and plaque control
- Stability of graft and soft tissue closure
- Adequate protection of the area during early healing
Adhering to post-operative instructions and maintaining a clean, stable environment around the grafted area support better outcomes and reduce complications.
Long-Term Maintenance After Bone Grafting and Implants
Once grafts have integrated and implants are in place, ongoing maintenance becomes the focus. Long-term stability depends on:
- Regular professional cleanings and evaluations
- Monitoring bone levels around implants with periodic imaging
- Controlling inflammation in the gums and peri-implant tissues
- Managing bite forces and wear on restorations
- Using nightguards when grinding or clenching is present
The same principles apply whether the case involves a single implant, multiple implants, or full arch reconstruction. A stable foundation created by effective grafting only retains its value when the environment around it stays healthy.
Summary
Bone health determines whether dental implants reach their full potential. Jawbone loss after tooth extraction is predictable and progressive, but bone grafting restores volume and shape so implants can anchor securely.
At JP Prosthodontics, grafting is never treated as an isolated procedure. It is integrated into a comprehensive plan that aligns prosthetic design, surgical steps, and long-term maintenance. Assessment, imaging, grafting, implant placement, and final restoration all follow a coordinated sequence aimed at durable, functional results.
For patients in Fullerton, CA who require advanced planning for implants, grafting, or full arch solutions, the starting point is a structured evaluation and a clear, staged roadmap built around the final outcome. Use the practice’s contact page to initiate that process and align bone health with long-term implant success.